Meniere’s disease is a chronic condition caused by increased fluid pressure in the inner ear and is characterized by vertigo, hearing loss, tinnitus, and a feeling of fullness in the ear. It usually begins in one ear and may lead to progressive hearing loss over time.
Attacks of Meniere’s disease typically last from several minutes to several hours. During an attack, imbalance and nausea are common. The disease can significantly limit a person’s daily life and social activities. Therefore, a multidisciplinary approach is necessary.
Although the exact cause is unknown, genetic factors, autoimmune mechanisms, and vascular abnormalities are thought to play a role. Salt intake, stress, and irregular sleep can increase the frequency of attacks. Therefore, lifestyle management is essential.
Treatment includes salt restriction, fluid balance, stress management, and medications. Surgical methods may be considered in advanced cases. Regular follow-up can slow the progression of hearing loss and reduce the severity of attacks.
Meniere’s disease is a chronic and progressive condition that causes permanent functional loss in the inner ear. Since this chronic condition significantly weakens the balance structures in the inner ear, individuals may experience balance problems severe enough to affect daily life. In such cases, these individuals need vestibular rehabilitation services provided by audiologists.
| Definition | A chronic disease characterized by vertigo, hearing loss, and tinnitus caused by increased pressure of the endolymph fluid in the inner ear. |
| Causes | – Problems with endolymphatic fluid absorption Genetic predisposition Autoimmune diseases Viral infections Stress and dietary factors. |
| Symptoms | – Severe and sudden vertigo attacks Unilateral hearing loss (initially often temporary) Feeling of fullness in the ear Tinnitus. |
| Duration | Vertigo attacks last between 20 minutes and several hours; symptoms usually decrease between attacks. |
| Diagnostic Methods | – Audiometric tests (to evaluate hearing loss) Tympanometry Videonystagmography (VNG) MRI (to rule out other causes). |
| Treatment Methods | – Medical Treatment: Betahistine, diuretics, antiemetics. Diet: Salt restriction, avoiding caffeine and alcohol. Surgical Intervention: Endolymphatic shunt surgery, labyrinthectomy (in advanced cases). Vestibular rehabilitation. |
| Who Is Affected? | More common in individuals aged 20–50; slightly more common in women than men. |
| Complications | Permanent hearing loss, decreased quality of life, psychological issues (anxiety, depression). |
| Follow-up and Recommendations | Stress management, regular monitoring of inner ear functions, dietary and lifestyle adjustments to reduce attack frequency. |
What Is Meniere’s Disease?
Meniere’s disease is a chronic condition associated with increased fluid pressure in the inner ear and is characterized by recurrent vertigo attacks, hearing loss, tinnitus, and a feeling of fullness in the ear. Attacks usually last for several hours and may be accompanied by nausea and vomiting. As the disease progresses, hearing loss can become permanent. Although there is no definitive cure, symptoms can be controlled through salt restriction, medications, lifestyle changes, and surgical methods in advanced cases.
https://www.youtube.com/shorts/8WY89BdY4rc
How Common Is Meniere’s Disease?
The prevalence of Meniere’s disease varies widely across different populations. Older individuals, white ethnic groups, and women are particularly affected. Several health conditions may accompany the diagnosis:
- Migraine: Migraine is more common among individuals diagnosed with Meniere’s disease.
- Autoimmune diseases: Rheumatoid arthritis, systemic lupus erythematosus, ankylosing spondylitis
Additionally, the theory that Meniere’s disease may have a vascular (vascular) origin has been discussed, although this theory has not yet been supported by definitive evidence.
Meniere’s disease also contains a genetic component. Approximately 10% of European individuals with this disease show familial transmission. Genetic predisposition may be inherited through autosomal dominant or recessive patterns, but in most cases it is sporadic. These genetic associations are an important research topic in understanding the disease. Studies on the genetic basis of Meniere’s aim to contribute to the development of treatment and diagnostic methods.
Factors such as stress and high salt intake are known to disrupt the balance of inner ear fluid. Additionally, abnormal fluid accumulation in the inner ear—called hydrops—is a prominent feature of Meniere’s disease. This fluid buildup causes hearing loss, vertigo attacks, and tinnitus.
What Are the Symptoms of Meniere’s Disease?
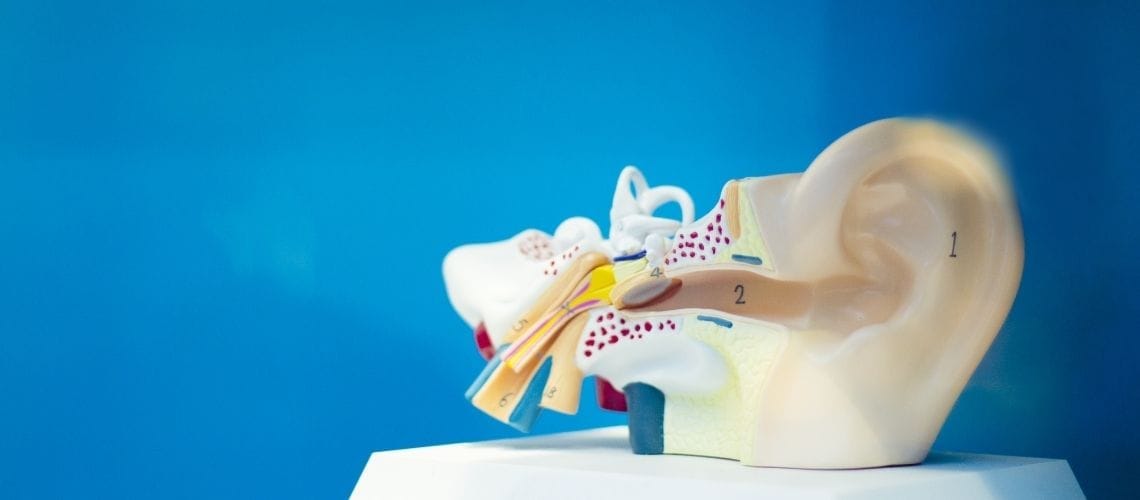
Meniere’s disease is a condition that affects the inner ear, causing significant problems related to balance and hearing. It is particularly characterized by three main symptoms: sudden vertigo attacks, hearing loss, and tinnitus.
- Vertigo Attacks: The most prominent symptom of Meniere’s disease is uncontrolled and unpredictable vertigo attacks. During these attacks, patients feel as if the environment is spinning. Attacks typically last for several hours and can cause severe balance problems and emotional distress.
- Hearing Loss: Hearing loss related to Meniere’s disease is usually unilateral. At first, the loss may be temporary, but as the disease progresses, it can become permanent. The observed hearing loss is more pronounced at low frequencies and is sensorineural.
- Tinnitus: Patients often report ringing or pulsating sounds in the ear. These sounds can be quite disturbing and negatively affect daily activities.
The symptoms are generally episodic, and patients may feel normal between attacks. However, after each attack, hearing loss may worsen and tinnitus may become permanent.
How Is Meniere’s Disease Diagnosed?
The diagnosis of Meniere’s disease is made based on patients’ described symptoms and audio-vestibular evaluations. The first step includes detailed hearing assessments (Pure Tone Audiometry, Tympanometry, and Acoustic Reflex Testing).
Additionally, high-resolution MRI is recommended for patients with unilateral hearing loss to rule out other possible inner ear pathologies. MRI can help visualize endolymphatic hydrops, the fluid accumulation specific to Meniere’s disease.
Vestibular function tests (Caloric Test, VNG, v-HIT, VEMP) are used in diagnosis. These tests evaluate the function of the balance-related sections of the inner ear, and significant functional loss is usually observed on the affected side.
These processes are critical for diagnosing Meniere’s disease and serve as the first step in its management. Each test is tailored to the patient’s condition, and comprehensive evaluation ensures accurate diagnosis. The information obtained from these tests forms the basis of the treatment plan.
What Are the Treatments for Meniere’s Disease?
Although a complete cure for Meniere’s disease is not possible, various treatment methods aim to reduce the severity and frequency of symptoms. These include dietary changes, medications, and surgical procedures.
- Low-sodium diet: Reducing sodium intake helps balance fluid pressure in the inner ear and reduce vertigo attacks.
Treatment options are individualized based on the patient’s condition and symptom severity. The goal is to improve quality of life while minimizing side effects. Therefore, patients should work closely with their doctors during treatment. Treatment requires a comprehensive strategy to slow disease progression and minimize daily discomfort.
What Other Conditions Should Be Considered in Meniere’s Disease?
Meniere’s disease is known for its specific symptoms of vertigo and hearing loss. However, other conditions with similar symptoms must be considered.
- Basilar migraine: Characterized by vertigo attacks with sensitivity to light and sound but does not cause hearing loss.
- Vestibular neuritis: Long-lasting vertigo episodes usually following an infection; however, hearing loss is not expected.
- BPPV (Benign Paroxysmal Positional Vertigo): Short vertigo attacks triggered by head movements.
- Central vertigo: Can be caused by stroke, multiple sclerosis, and other neurological conditions.
- Non-otogenic peripheral vertigo: More common in elderly individuals and usually related to neuropathy.
- Orthostatic hypotension: Not classified as vertigo but causes dizziness.
- Neoplastic and infectious causes: Including vestibular schwannoma, meningioma, and meningitis.
https://www.youtube.com/shorts/Xj8kWdcnbKQ
What Are the Complications of Meniere’s Disease?
Meniere’s disease is a progressive condition involving the inner ear and can lead to various complications. As the disease advances, individuals may experience Tumarkin’s crises—characterized by sudden falls without loss of consciousness due to loss of muscle tone. Additionally, people with Meniere’s disease report decreased quality of life compared to the general population. Psychological effects include increased anxiety levels and depression.
Individuals with Meniere’s often struggle due to these health challenges, which negatively impact daily life. The uncertainty caused by the disease and factors such as hearing loss increase psychological burden and complicate social and professional life. Understanding these complications and receiving appropriate support is essential for coping with the disease.
Frequently Asked Questions
What exactly causes Meniere’s disease?
The exact cause is unknown, but fluid buildup and increased pressure in the inner ear are the main mechanisms. Genetic predisposition, autoimmune processes, and infections may also play a role.
Who is more likely to have Meniere’s disease?
It typically appears between ages 40–60 and is slightly more common in women. Individuals with family history, migraine, allergies, or autoimmune diseases have higher risk.
What happens during a Meniere’s attack?
Sudden vertigo, pressure in the ear, tinnitus, and hearing loss occur. Attacks may last from minutes to hours and may be accompanied by nausea and vomiting.
Is hearing loss permanent in Meniere’s disease?
Initially, the loss fluctuates and may partially recover between attacks. However, as the disease progresses, hearing loss becomes permanent and more pronounced at low frequencies.
How does Meniere’s disease affect daily life?
Frequent vertigo attacks hinder work, social life, and family interactions. Individuals may develop fear of falling, anxiety, and depression, significantly reducing quality of life.
Why are diet and lifestyle important in Meniere’s disease?
Salt restriction and reduced caffeine/alcohol intake help maintain inner ear fluid balance. Regular sleep, stress management, and avoiding smoking reduce attack frequency.
What does drug therapy achieve in Meniere’s disease?
Diuretics, vestibular suppressants, and anti-nausea medications reduce the severity and frequency of attacks. While medications do not cure the disease, they help maintain control.
When is surgery considered in Meniere’s disease?
If attacks cannot be controlled despite medication and lifestyle changes, surgical options such as endolymphatic sac surgery or vestibular nerve section may be considered.
How is Meniere’s disease supported with vestibular rehabilitation?
Meniere’s causes functional imbalance. Although many patients focus on attack control, improving balance ability is equally important. Vestibular exercises strengthen balance structures and improve quality of life. Recovery after attacks becomes easier, and daily adaptation improves.
Is Meniere’s disease completely curable?
Meniere’s disease is chronic and progressive. As with all chronic diseases, slowing progression is the primary goal. Although there is no definitive cure, symptoms can be managed with medication, lifestyle changes, and surgery. Vestibular rehabilitation helps improve balance. The goal is managing the disease and protecting quality of life.

Dr. Audiologist Emel Uğur was born in 1982 in Çanakkale. She specialized in Pediatric Audiology, Otologic Disorders, and Vestibular System Disorders, and served for 15 years at the Istanbul Training and Research Hospital. In 2015, she joined the Acıbadem Healthcare Group. She currently works as an Audiologist at the Acıbadem Altunizade Hospital and also serves as a faculty member and program director in the Acıbadem University Vocational School of Health Services Audiometry Program.








Location of our clinic in Istanbul, Turkey